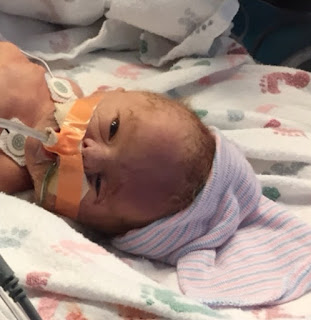
Jude’s Birth Story - Part One
At 5 am on Monday, September 14th I began having
what I thought were Braxton Hicks. Just in case, I began timing them on an app
I had on my phone. About a week prior I had the same experience, but when I got
out of bed they went away. I assumed these would do the same, and being so
tired, I just stayed in bed and slept in between each contraction. The
contractions stayed consistent at about 30-seconds long every 15 minutes, so I
did not worry too much about them being the real thing because they were not
progressing in any way.
Around 8:30 I got out of bed thinking that the contractions
would just go away. I went to the bathroom, and a large dark-green discharge
came out (sorry, TMI) which we later learned to be the baby’s meconium. I immediately
called Beth, who has been doing my ultrasounds in Denver since our first
appointment at Children’s Hospital Colorado months ago and told her what was
going on. She let me know it was all going to be okay, and told me she would
call the hospital, since she was off that day, so they would know I was on my
way. By what I believe to be inspiration, my sweet friend Reagan had been
visiting over the weekend and I left the bathroom franticly and told her what
had happened, that I had been having contractions, and that we needed to go to
the hospital.
I started to panic, realizing that I would be having the Jude
that day. Reagan was so calming and reassured me it would all be okay. We
quickly left the Ronald McDonald house where I had been staying over the last
few weeks, I called Vahe (who was already driving to the airport for a
pre-planned visit) to let him know what was going on, and we drove to the
hospital. On the way, I asked Reagan to say a prayer and in all of my fear and
anxiety and panic I felt a sense of peace and comfort in knowing that I was
continuing to be watched over.
When we got to the hospital, my nurse Jenn met us in the
hallway. I remember hugging her and crying and telling her I was scared – at
this point I knew most of the nurses on the unit pretty well. She tried to calm
me down and took me to the room that they had ready for me, since Beth had
already called to tell them I was on my way. By this time my contractions were
stronger and closer together – I assumed just because I was panicking and so
stressed out. I had no idea that I was so far along in labor.
Dr. Galan and Dr. McGloughlin came into the room soon after.
Dr. Galan checked my cervix, I was completely dilated. They let me know that
things would be moving very quickly, and that Jude would be born very soon. I
remember feeling like I was in shock.
Of course I would have wanted to have Vahe by my side more
than anything, but it was such a blessing to have Reagan there with me – a
sweet mother of four, who knew exactly what I needed to hear to help reassure
me everything would be alright. She held my hand and stroked the hair out of my
face and was the perfect nurturing and loving presence that I needed at that
time. She told me it would all be okay.
The doctors and nurses suited up for the operating room, and
Reagan was given a suit so she could come in with me. They told her that she
would just need to wait outside until after my spinal was in. I handed her my
phone and asked her to take pictures.
Within minutes we were in the operating room. The doctors
were very torn as to whether or not to delivery vaginally or by c-section,
because Jude was already half way out. He was breech, but they thought that if
they could deliver vaginally and get his belly out that they would not have any
other problems. They asked me to push. I pushed three times and Jude did not
move. His heart rate began dropping and so they quickly decided to do a
c-section. They sat me up to do a spinal, and Jude’s heart rate dropped again, dramatically.
So, they laid me back down and put me under general anesthesia.
I was very nervous to go under, mostly because if Jude only
had a few minutes to live – I wanted to be there to witness life in my baby
boy. In the end though, due to the severity of the c-section, I was very
grateful that I was not awake during the procedure.
Apparently, a technique in trying to minimize the chance of
aspirating when under general anesthesia is to press on a certain point on the
patient’s throat. Although we later joked about it with our nurses, I truly
believed that when they were initially putting me under – and holding my throat
very firmly, that they were just trying to knock me out quickly by limiting my
air supply. I remember asking the nurse holding my throat if she was trying to
choke me out, but I think I was asleep before I could even worry about it.
Because I was put under general anesthesia, Reagan was not
allowed to come in for the delivery. The doctors told me that they attempted a
normal c-section, but Jude was stuck in the birth canal. Because of this, they
made an additional upward incision laterally, basically creating a T shape so
that they could pull him out at a better angle. Unfortunately, in trying to get
him out, my uterus also tore completely down as well – essentially, my uterus
was open flat. Because of this, it took them 2 ½ hours to stich me up and move
my bladder and intestines back to the right place. For this reason, I am so
glad I was not awake – I am sure I would have panicked in wanting to see Jude
and to know if he was okay, or even alive, the entire time.
Reagan not being able to come into the delivery was another
blessing in disguise because she was advocating for me the entire time, while
also keeping Vahe and my family updated. She got to see Jude as they brought
him out and started trying to get him to breathe. She took the only pictures
that we have of him with his eyes open, while I was still in being stitched up
and Vahe was still on the plane, which will always be a treasure and blessing
for us to have. At one point before Vahe or I were there, the doctor thought
that Jude may only have minutes to live, and Reagan was able to call and
communicate with Vahe what was going on - fortunately, Jude pulled through.
When I woke up from anesthesia around 12:30, Vahe was the
first person that I saw. I was so relieved to see him, and my heart felt so
calm knowing that he was there with me. Not realizing that I had been out for
so long though, I was very surprised that he was there. He told me that he had
just arrived at the hospital from the airport only minutes before, and
explained that I had had a complicated c-section and had been under for a few
hours.
Through the cooperation of both my doctors and the NICU, a
NICU room was cleared out as a recovery room for me directly across the hall
from Jude, the first time they had ever let an adult patient in their unit.
They wheeled me into the room, and I remember being more
nauseated then I ever have in my life. I was so sick, and in so much pain. I
asked if Jude was alive. Vahe told me that he was and pointed out that he was
in the room across the hall.
I could see in the room, but there were so many machines and
nurses around that I couldn’t see Jude. But, I knew that he was in there and
close to me. And I knew he was alive. Not seeing any sense of urgency among the
nurses and doctors working on him was a great comfort.
They let me stay in the NICU room until Jude was stable
enough to go in to see him. I remember being so anxious to go in. Around 5:30
pm they wheeled my bed into his room.
The nausea and pain seemed to just go away when I saw that
perfect baby boy. He had so many tubes and wires all over him, but he was so
beautiful. His skin was pink and warm. He was on an oscillator to help him
breathe, so his chest was moving up and down quickly. But he was breathing. His
arm was extended toward me and I put my finger in his hand. After a minute or
two of just holding his hand, he squeezed my finger. I will never forget that
moment. It was the only time I felt his warm body move, being so alive –
perhaps telling me in that one gentle motion that he was okay.
Those few minutes that we spent with Jude seemed to go by so
quickly, but I am so grateful for them. Since Jude was stable, and I was still
recovering, they took me back to my room. Reagan says she remembered it being around 6:00 when we came back to my room on the MFM floor.
It must have been just an hour later that Jude’s doctor came
in to give us an update on him. She explained all of the procedures that they
had done, and how they were able to get him to breathe. At this point I was
still pretty heavily medicated, so I have a hard time remembering the details –
all I remember was that my baby boy was alive, and that they were optimistic that
he was going to pull through. She told us that although
during the first few hours of his life they did not think that he would make
it, that since then – he had been doing progressively better. She was
optimistic that he would be okay, and told us that he was in a “critically
stable” condition.